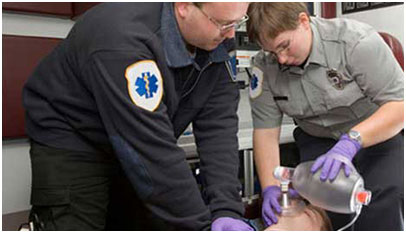
Dispatch-Assisted CPR
Ensuring that local dispatch centers provide the most effective dispatch-assisted CPR instruction is the best way to improve bystander CPR in any community.
Emergency Medical Dispatch (EMD) is a vital component of any Emergency Medical Services System. An EMD program should provide written, medically approved guidelines or protocols that emergency medical dispatchers use to effectively deliver pre-arrival emergency telephone instructions, including CPR. The assistance to provide CPR instructions and walk the caller through the delivery of CPR for the patient is known as Dispatcher Assisted CPR.
Time from collapse to initiation of CPR is a critical factor in determining survival from out-of- hospital cardiac arrest. Providing CPR instructions over the telephone immediately after someone calls 911 is a critical element that decreases time from collapse to initiation of CPR. The response time for most EMS systems in the United States is 4-6 minutes. An assertive and well trained dispatcher can recognize cardiac arrest and have the bystander performing CPR in less than 1 minute from the time the call was received. Studies have shown that DA CPR can improve the percentage of cardiac arrest cases that receive bystander CPR and overall survival.
Helpful Links
- Seattle and King County’s Resuscitation Academy’s resource section on Dispatch Assisted CPR
- Arizona’s SHARE Program resources on Dispatch Assisted CPR
- Circulation 2012: A Scientific Statement from the American Heart Association on Pre-Hospital Arrival
- Circulation 2001: Dispatcher assisted cardiopulmonary resuscitation and survival in cardiac arrest
High-Performance CPR
EMS systems should train to provide high-performance resuscitation. This includes a well-planned, well-rehearsed, often choreographed and flawlessly executed approach to caring for the victim of SCA at the scene.
The goals of high performance resuscitation include the provision of continuous, high-quality CPR, rapid defibrillation, non-aggressive airway placement, and the use of end tidal CO2 wavef-rm to both confirm tube placement and monitor the quality of the resuscitation efforts. Systems should have clear termination of resuscitation protocols, which allow the patient to receive the most complete care possible at the scene prior to termination of efforts.
Following the resuscitation, a post-event review should occur as soon as possible using all available quality improvement tools available. A review of system dispatch times allow crews to determine if quicker response is possible. Review should also include a determination of whether or not bystander CPR was provided by dispatch evaluation of CPR fraction and quality of compressions if possible, evaluation of ventilation rate and end tidal CO2 waveforms and appropriateness of all treatments provided in the field. Having crews and medical directors implement adjustments and improvements to these system components following review of the event constitutes a high performance resuscitation program.
Helpful Links
- Seattle King County’s Resuscitation Academy has many resources, including a section on high performance CPR
- The American Heart Association Guidelines for CPR and ECC